INTRODUCTION
The popularity of dental implant treatment has increased exponentially over the past few years. Even though people are enjoying better dental health, tooth loss is still common. Today, people are living longer and expect to remain active well beyond their sixties and into their seventies. Having the ability to smile with confidence and to eat their favorite foods forms part of these expectations for a long and happy retirement.
With an aging population that includes the baby boomer generation, the demand for long-term solutions for tooth loss is set to grow. Figures from the AAID show that currently 3 million people in the United States have dental implants, a figure that is growing by 500,000 annually. By 2022, it is estimated that the implants market both in the United States and in Europe will be worth $4.2 billion. Patient demand for dental implants is increasing, in part due to public awareness about this service and the fact that it has one of the highest success rates in dentistry at a rate of 95% or more.
During this same period, dental implant technology has also moved forward with the introduction of newer techniques and materials that increase the predictability and reliability of implant treatment. CADCAM technology and 3D printing are set to transform the market during the next few years. Today’s clinician must consider many different factors when deciding which implant systems they will offer their patients and which techniques will be most valuable in their practice.
IN THIS GUIDE WE WILL DISCUSS:
- The most popular implant systems amongst dentists
- Types of implants
- Pros and cons of using model-less restorations
- Benefits of using CT scans
- Surgically guided implants
- Full zirconia implant-retained prosthesis
CHAPTER I: THE MOST POPULAR IMPLANT SYSTEMS AMONGST DENTISTS
Dental implants come in a variety of shapes and sizes which have evolved to improve treatment and to fit in with current surgical techniques.
The top dental implant companies are continually researching how making subtle changes to the surface texture, shape, width, and length of implants could affect and improve success rates.
WHICH COMPANIES MAKE THE MOST POPULAR IMPLANT SYSTEMS?
Although well over 100 companies produce implant components, there are just a handful of major dental implant companies that are well-known and well-respected worldwide.
These companies include:
Straumann, Zimmer Biomet, Nobel BioCare, MIS, BioHorizon, and Dentsply.

WHY CHOOSE ONE OF THE MOST POPULAR IMPLANT SYSTEMS?
While there are numerous generic implant companies that may offer cheaper components, this can prove to be a false economy. First, patients are becoming increasingly well educated about dental implant technology and are more likely to demand their chosen dental implant dentist uses a well-known manufacturer for their dental implant treatment. Having documented evidence showing the provenance of implant components and restorations can help a patient choose their implant dentist.
Secondly, any decent dental laboratory will be familiar with these top manufacturers and their technicians will have the specific training and tools to use the required components. Thirdly, it’s a great selling point for practices to offer dental implants made from one of the top companies, particularly as we continue to move even closer towards becoming a global economy where people will frequently need to relocate to a different country. Knowing they can easily maintain or replace dental implant components wherever they might be in the world provides valuable peace of mind.
GAIN BENEFIT FROM YEARS OF DOCUMENTED RESEARCH
The top implant companies have invested heavily in research and development. By choosing their products, you are assured you will be receiving top quality with long-lasting components. Extensive research has been carried out into surface characteristics of dental implants. When the implant is first placed in the body, it promotes a biological response leading to an exchange of information between cells and biomaterials at the point of contact.
This induces either acceptance or rejection of the dental implant and will determine how many cells will populate the implant surface. It has been shown that osteoblastic cells can adhere more quickly to roughened surfaces compared to smooth surfaces, a quality that top dental implant companies have focused on in order to promote better osseointegration.
The biomechanical qualities of dental implants manufactured by the top companies will have been clinically researched with the results available for everyone to view. In comparison, the biomechanical qualities of generic dental implants can be an unknown quantity, however closely they may replicate a brand manufactured implant.
DECIDING WHICH IMPLANT SYSTEMS TO USE
Deciding which implant system to invest in can be a bewildering and time-consuming process. For most routine implant cases, it is less likely to matter which implant system you choose but your choice of implants can become more relevant in more complex situations such as for patients with low bone volume.
When selecting your implant system, it’s worth reviewing their websites so you gain an overview of their products, before scheduling any meetings with sales reps. Today, most dental implant companies strive to become a one-stop resource, producing all the implant components you are likely to require as well as other professional dental care products. However, if you intend for dental implants to become an integral part of your practice, it is unlikely that one system will always be able to accommodate all your patient’s needs. You might need to consider at least two different brands to cover your clinic’s potential requirements. Generally, it can be better and easier for a practitioner to deal with a fewer number of manufacturers and it makes sense to spend some time getting to know a particular dental implant system extremely thoroughly when first introducing this service for your patients.
CHAPTER II: TYPES OF IMPLANTS
Once you have decided your implant systems, you will need to choose when to use cement-retained abutments or screw-retained implants, and when to choose custom abutments instead of stock abutments. Generally, for better esthetic results, a custom abutment is often recommended but this can vary from case to case.
Although many dentists prefer titanium implants, zirconia is becoming more popular. Then, there are the different types of crowns that can be used when placing a custom abutment.
CEMENTABLE ABUTMENTS VERSUS SCREW-RETAINED IMPLANTS
When choosing whether to supply cement-retained implant crowns or screw-retained implant crowns, there are various factors you will need to consider. These factors include retrievability, how well it will maintain the peri-implant tissues, how easy it will be to use, whether it is suitable for use with angled implants, and last but not least, the cost.
RETRIEVABILITY
Sometimes it is necessary to temporarily remove an implant crown. There are certain cements on the market that are made specifically for implant restorations which claim the implant crown will be easy to retrieve. Some dentists may also use temporary cement to hold implant crowns in position. This can be a good solution but it does mean that the crown will be less retentive which is less than ideal. In comparison, a screw-retained implant crown is far more predictable if the crown needs to be retrieved, particularly when a greater number of abutments are required. A multi unit restoration that is cemented in place will be far more difficult to predictably remove.
MAINTAINING PERI-IMPLANT TISSUES
When a crown is cemented into place there is always the danger that excess cement could be extruded into the sulcus. When this is the case, it can damage the peri-implant tissues unless the cement is fully removed. When subgingival cement is present around an implant, it can increase the risk of peri-implant mucositis and peri-implantitis. While there are good techniques for removing subgingival cement when placing an implant crown, there is still a risk that some cement may be missed. In comparison, a screw-retained crown doesn’t carry this risk and may be easily removed for maintenance and cleaning.
EASE-OF-USE
Inserting a screw-retained implant crown can be more challenging compared to a cement-retained crown. This is particularly the case when fitting multiple unit restorations. With a cement-retained restoration where multiple abutments are required, the procedure to fit the restoration is still quite similar to a routine bridge placement. In comparison, placing a screw retained restoration requires a number of extra steps to ensure the framework has passive fit, and ideally, the restoration should induce no stress on the implant.
SUITABILITY FOR USE WITH ANGLED IMPLANTS
For esthetic reasons, it is not possible to place screw holes in the incisal or facial contours of implant crowns. If the implant angle is slightly incorrect, then it is necessary to use an angled, screw-retained abutment which increases the cost. In this case, it is much easier to rely on a cement-retained crown using either a custom abutment for a stock angled abutment.
STOCK ABUTMENTS VERSUS CUSTOM ABUTMENTS
For each implant case, you will need to decide whether to use a stock implant abutment or a custom implant abutment. To make the right decision, it is worth being aware of the features of each option so you can make the best choice for your patient.
WHEN TO CHOOSE STOCK ABUTMENTS
Stock abutments are standard sizes and may be used for bone level and tissue level implants. Dental implant companies have designed stock abutments to be user-friendly, making it possible to easily take impressions. Stock abutments tend to be used for cement retained restorations and are often an economical choice. You can choose between angled and straight abutments, and stock abutments are best used for tissue level implants that are not within the esthetic zone.
One problem with stock abutments is because they are standard size, the tissue will conform to the shape of the abutment. This is why these abutments are not an optimal choice for use within the esthetic zone as it is more difficult for a ceramist to create the correct emergence profile, providing vital tissue support and optimal results. Another thing to consider is that with stock abutment it is not possible to control the final margin placement of the crown, as this is determined by the depth of the implant and the height of the abutment. You may need to spend more time making chairside alterations in order to get the correct fit and emergence profile.
WHEN TO CHOOSE CUSTOM ABUTMENTS
Custom abutments are suitable for either bone level or tissue level implants and may be waxed or milled into precisely the right shape relative to the crest of the tissue. There are several different types of custom abutments that may be made from titanium or zirconia, or will be fabricated from zirconia with a titanium base. When placing a custom abutment, the use of delivery jigs helps ensure the restorative process is smoother and more accurate, saving valuable chairside time. One aspect to consider with custom abutments is that although they are more expensive, they can provide more predictable esthetics and superior tissue management. They can be suitable for both screw retained and cemented crowns. Clinically, custom abutments can be more efficient than stock abutments, making them a more cost-effective option as you will save on lab fees in modifying stock abutments and on clinical resources during fitting.
WHY MOST DENTISTS PREFER TITANIUM OVER ZIRCONIA
TITANIUM IMPLANTS
Most dental implants are made from titanium, a material with proven biocompatibility that integrates with bone extremely well. Bone is able to grow on the surface of titanium dental implants, making them immovable. The success rates for titanium alloy implants is typically 95% or even higher. Initially, pure titanium was used to fabricate implant components but was found to be too soft, which is why implant companies developed an alloy capable of offering superior strength while still retaining excellent biocompatible properties. Although there haven’t been any cases of allergic reactions to titanium, very occasionally some people may be particularly allergic or sensitive to other metals used in the alloy. Around 5% of people have a nickel sensitivity or may have other concerns about having anything metal in their body.
ZIRCONIUM IMPLANTS
Due to concerns about possible sensitivities and allergies to titanium alloy, some companies have researched and developed metal-free implants using zirconium. Although this material is called a ceramic, it does contain trace amounts of two other metals, hafnium, and yttrium which helps to improve its properties. Zirconia is extremely strong and it osseointegrated in a similar way to titanium.
PROS AND CONS OF EACH MATERIAL

Titanium is proven to be successful in implants that are still functioning well after decades of use. It is possible zirconia will be equally successful but at the moment, long-term success rates are not available. Titanium implants are more versatile because they are fabricated as one or two-piece systems, allowing dentists greater flexibility in planning treatment and in surgical placement. The options for use are greater as titanium implants may be used to support fixed restorations, as well as overdentures.
Zirconium implants are fabricated in a single piece so implant restorations must be cemented in place. Greater care needs to be taken when placing these implants and bone volume is particularly important because there is so little room for error. However, there are several advantages of using zirconia dental implants, as the material is thermally non-conductive and it will not corrode. The ceramic color of the material ensures there is no risk of metal showing at the gum line, but the possibility of this happening with titanium implants is rare.
In most cases, using titanium dental implants will provide reliable results backed by years of research and development. Titanium implants provide a more flexible approach to treatment that may ultimately produce better results for the patient. However, if a patient has real concerns about using metal implants, zirconium could be a useful alternative on occasion, provided the patient understands the possible limitations of this treatment.
TYPES OF CROWNS TO USE WHEN PLACING A CUSTOM ABUTMENT
Crowns that may be used when placing a custom abutment include PFMs, e-max. full gold, and zirconia which may be layered or full-contoured. PFMs and full gold crowns are the most reliable choice since even, temporary cement can be used to hold them in place. Both are good options where space is limited since PFMs can be constructed with metal bite stops where the patient’s bite is particularly heavy, or where they may be opposing another implant crown. Esthetics may be one disadvantage of using PFMs, particularly around the gingival margin.
Lithium disilicate or e.max crowns can make very successful restorations for zirconia custom abutments. Using resin cement with these crowns reduces the risk of fracturing. One problem with using resin cement is its translucency and low viscosity which can make it difficult to ensure no cement remains sub-gingivally. As a result, resin cement should not be used where the margin is more than 1mm subgingival and is only recommended if additional strength is needed from an e.max crown.
Full contour zirconia crowns can be very successful, but there is no long-term literature into their effect on tooth enamel. Wear on opposing teeth from full zirconia is not yet clear. Layered zirconia crowns require greater occlusal clearance compared to full-contour crowns. Aesthetically, all-ceramic crowns can provide the highest standards of restoration but this does rely on the technician’s skill in using these materials.
Ultimately, your choice of crown will depend on the type of custom abutment chosen, the location of the abutment, and the patient’s personal preferences.
More helpful links:
Minimizing the risk of dental implant complications »
Zirconia Dental Implants - Pros and Cons »
Fixed implant bridges: Treatment Details »
Advantages of Zirconia implant abutments »
Tooth Replacement: Implant versus bridge »
Screw-retained implant crown »
When to use narrow diameter dental implants »
CHAPTER III: PRO’S AND CON’S OF MODEL-LESS RESTORATIONS
Traditionally, a good dental impression is an essential component in achieving a great restoration but the margin for error when taking a conventional impression is considerable. Both clinical skill and experience can affect the quality of the final impression. Inadequate impressions are often associated with bleeding or may be due to the limitations of impression materials.
Over the past few years, the introduction of digital technology has begun to revolutionize dentistry, helping to eliminate many of these problems through the use of intraoral scanners. These newer systems avoid the use of traditional dental impressions, instead collecting digital data for the fabrication of precision restorations. Digital impression files commonly accepted by dental labs include Sirona CEREC®, 3Shape TRIOS®, Carestream®, and ITero® but a good dental laboratory should be able to cope with files from any open system.
Originally, some of these systems would only scan a portion of the mouth but many have since expanded their capabilities to become full mouth scanners. Each intraoral scanner works in a slightly different way to capture the data.
For example, Sirona CEREC® uses triangulation to collect images, where a light source is reflected off an object and a sensor detects depth-dependant changes in the light. To increase the accuracy of the image, the surfaces to be scanned must be coated with a reflective, opaque coating. Sirona does not require surfaces to be coated, instead collecting white light video to create an image of the tooth. ITero® uses a parallel confocal system, filtering light through a pinhole so that only light reflected at the correct focal distance will pass back through the pinhole.
Two questions asked by many clinicians are:
“What is the outcome of using these new systems?”
“Which materials and restorations can be utilized?”
Digital impressions sent to a dental lab can be used in two different ways. One option is to use these impressions to create polyurethane or resin models that can then be utilized to fabricate restorations using conventional laboratory processes. These processed digital models can be used to wax-up cast metal restorations or substructures which can then be finished conventionally. The second option is for digital impression data to be used directly by inputting the information into a CAD/CAM program. This data can then create computer graphic designs of full contour restorations or designs for substructures.
The most common use for digital impressions is to create zirconia crowns and e.max restorations. Utilizing e.max® and Zirconia HT is a particularly popular solution due to the material’s excellent flexural strength.
By combining digital and traditional processes, it is possible to create gold or PFM crowns in a way that is highly dependable which should produce well-fitting restorations with an excellent marginal fit.

WEIGHING THE PROS AND CONS OF MODEL-LESS RESTORATIONS
COST
Cost is likely to be a major consideration when purchasing digital scanning technology as the expense needs to be reclaimed with increased profits, or by decreasing costs. Model-less restorations will produce savings in impression materials, supplies and lab bills.
PATIENT COMFORT
Patients often prefer this technique, particularly those with a strong gag reflex or individual with a small mouth because it provides a far more comfortable experience. Scanning can be paused at any time, allowing the dentist to remove saliva and blood before resuming.
ACCURACY
There have been several clinical studies into the accuracy of digital impressions compared to conventional impressions. Model-less restorations have been found to provide a high degree of accuracy equal to or better than conventional impressions, and crowns may have a better marginal fit. Additionally, digital impressions can measure the occlusal clearance between opposing teeth. Sending digital files to your dental laboratory will enable you to gain better results through improved communication with your dental lab. However, digital impressions do require that the entire margin is exposed as well as 0.5mm of tooth structure apical to the margin. This helps ensure a good emergence profile can be created in the dental lab.
TIME
As the files are sent digitally, it can help shorten laboratory times. Digital impressions can potentially be quicker once you become thoroughly familiar with the technology as there is no need to select the correct tray, prepare the tray or disinfect impressions. The accuracy that can be obtained with digital impressions should result in fewer remakes and less time spent chairside adjusting restorations to fit. Having the ability to see the scan on-screen makes it possible to monitor the quality of the preparation. If any inadequacies are noticed, then the area can soon be rescanned as opposed to spending time preparing and retaking a conventional impression.
COMPATIBILITY
Different systems have very different capabilities so it is important to choose the system that fits in with your practice requirements. Some digital impression systems are integrated with 3D imaging, allowing you to create fabrications over implants. Others have the capability of scanning healing caps over implants, enabling a dental app to fabricate custom abutments and crowns. These technologies could be extremely useful for a practice already routinely placing dental implants or for an office that is looking to expand their dental implant services.
TRAINING
Evaluating the training provided with your chosen system is another important consideration. Some companies will provide onsite training for a limited number of clinicians and assistants. Others provide training at their head office. Initially, onsite training may seem a preferable option but training at the headquarters of your chosen system allows you and other staff members to absorb all the information without distractions.
CHOOSING A SYSTEM THAT WILL GROW WITH YOUR PRACTICE
All these systems require a considerable investment so it is worth considering which can grow with your practice. For example, you might not currently offer orthodontics but if you intend to include this service in the future, it can best to choose a system that will be compatible. Every system has its benefits that will appeal to practitioners such as the method of scanning, the size of the wand, the ability to capture color or full-mouth scans, and ease of using the software. It is worth investigating several systems to see which feels the most comfortable to use and which has the features most required for your practice.
There is little doubt that model-less restorations can represent a substantial investment for any dental practice. However, this technique can provide a more comfortable patient experience, may reduce chairside time, and will produce well-fitting restorations.
More helpful links »
Paralleling technique in dental radiography »
Benefits of digital impressions »
Digital Impression Systems: Which scanner is right for you? »
How to achieve best results with a dental implant impression »
How to send a digital impression »
CHAPTER IV: THE BENEFITS OF USING CT SCANS
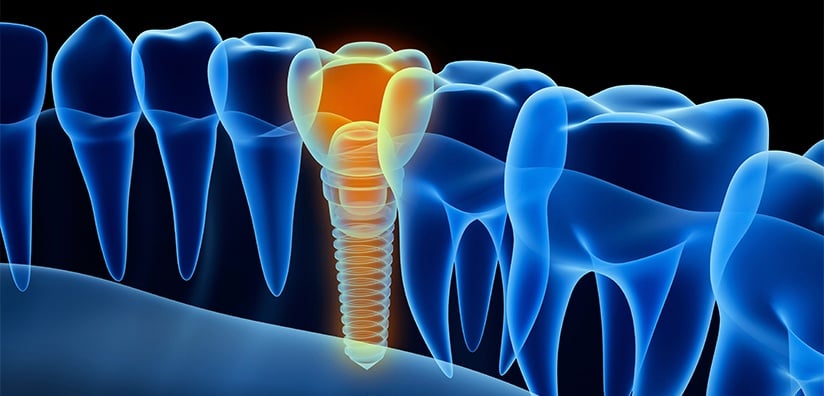
The introduction of more affordable cone beam CT scanners has prompted a growing number of dental practices to invest in this technology. Those who have not will often choose to send patients to clinics offering this service.
Cone beam CT (CBCT) scans are useful for procedures which include:
- Endodontics
- Oral surgery
- Orthodontics
- TMJ
- Diagnosing and treating impacted teeth
- Diagnosis and placement for dental implants
- Surgical guide fabrication for implant treatment
Radiation doses are approximately 15 times lower compared to conventional CT scans and an increasing number of practitioners believe the tiny risks posed by radiation exposure are far outweighed by the potential benefits. Imaging modalities enable clinicians to see a true representation of a patient’s maxillofacial skeleton and an image can be taken in a relatively short amount of time. Most practitioners will only carry out some procedures where the use of a CT scan is helpful. Many practitioners will have managed adequately without using CT scans and may be hesitant about investing in this technology and the training required to fully utilize it.
ADVANTAGES OF USING CBCT SCANNING IN IMPLANTOLOGY
 CBCT imaging gives the ability to view comprehensive data and to manipulate that data because many machines offer options for selecting different fields of view. This is particularly useful for dentists planning implant surgery. A CBCT scan immediately allows anatomical features to be accurately located and enables the shape and size of the ridge to be closely assessed. A clinician can easily see if there is sufficient quality and quantity of alveolar bone. It also detects pathology that must be avoided during implant surgery which includes the exact position of the nerves and the position of the submandibular fossa.
CBCT imaging gives the ability to view comprehensive data and to manipulate that data because many machines offer options for selecting different fields of view. This is particularly useful for dentists planning implant surgery. A CBCT scan immediately allows anatomical features to be accurately located and enables the shape and size of the ridge to be closely assessed. A clinician can easily see if there is sufficient quality and quantity of alveolar bone. It also detects pathology that must be avoided during implant surgery which includes the exact position of the nerves and the position of the submandibular fossa.
The images are very useful when planning implant placement and identifying the need for bone or sinus lifts. Clinicians can choose the appropriate implant size, the best location, and angulation. If necessary, they can change the trajectory of an implant to accommodate bone deficiencies or can plan to augment the site. Using special software, it’s possible to carry out virtual surgery, enabling dentists to thoroughly evaluate the quality of bone through dimensions and density shading. Advanced planning can be utilized to produce a surgical guide or stent for surgery. CBCT scanning is also helpful in allowing dentists to illustrate implant treatment plans to patients, facilitating better patient understanding along with greater acceptance of treatment. With a CBCT scan, clinicians can sit down with patients to discuss treatment including possible limitations. Additionally, it is possible to produce a wax-up or virtual images of implant teeth so patients can view the predicted results and are fully aware of the treatment outcome.
With the use of this technology, dentists can gain patient trust and help reduce completion time while enhancing the chances of implant success. It is worth remembering that in just a single scan, CBCT devices can also be used for more traditional radiography, providing panoramic, cephalograms and 3D images.
Helpful link:
3-D Cone Beam scanning techniques »
CHAPTER V: SURGICALLY GUIDED IMPLANTS
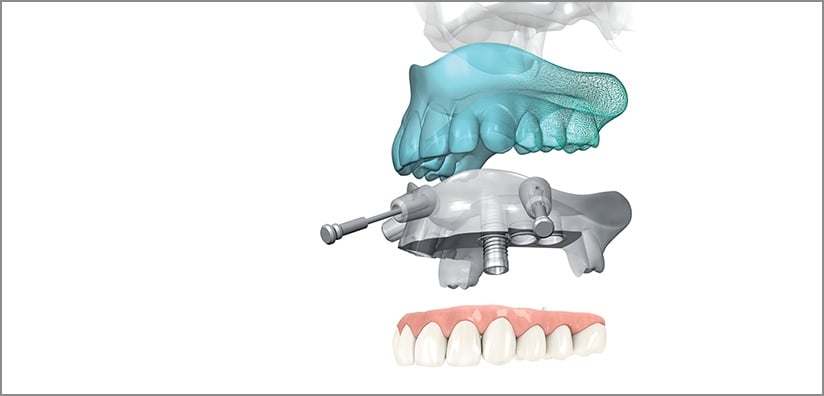
Surgically guided dental implants provide dentists with the opportunity to virtually plan implant surgery before placing the implant in the most accurate and predictable manner available. With guided surgery, it is also possible to place implants in optimal esthetic positions by using the software to superimpose abutments, allowing the room required for implant restorations to be more accurately calculated.
Using a surgical guide is one of the safest ways to perform implant surgery, as the guide will rest on bone, gingiva, or teeth. A guide will also have stops limiting the depth of the drill and the depth of the implant. These aspects effectively eliminate the guesswork in implant surgery, allowing you to accurately replicate your surgical plan without any deviations. Surgically guided implants can be particularly beneficial where space is limited, where angled implants are required, and in cases of immediate placement and provisionalization.
CREATING A SURGICAL GUIDE
When creating a surgical guide, it is necessary to produce a diagnostic wax-up which is replicated to create a radiographic guide that has radiopaque markers. The wax-up is worn by the patient during their CBCT scan and a second scan is taken using just the radiographic guide. The data is then used to plan implant placement and can be converted by the dental lab into an actual surgical guide using the scan of the radiographic guide for reference. One advantage in using a radiographic guide is the ability to see the potential implant positions and restorative implant positions in an overlay of the CBCT scan.
ADVANTAGES OF SURGICALLY GUIDED IMPLANTS
If all the steps have been correctly carried out, then surgery should be fast and accurate, yielding predictable results. Advance planning with the use of a surgical guide also helps to provide a more comfortable, minimally invasive experience for the patient, potentially shortening the appointment time and aiding with faster healing since only very limited incisions are needed. Lastly, it can also be less stressful for the clinician.
POSSIBLE LIMITATIONS OF SURGICALLY GUIDED IMPLANTS
A surgical guide will only be as good as the virtual or actual impression. Your dental lab is reliant on you taking an accurate impression. Although they can alert you to obvious faults, these may not always be visible in the dental lab. Carefully checking your impression while the patient is still in the chair will help to reduce this margin for error. Fabricating a surgical guide will also incur additional lab costs, require more time for planning the guide, and in communicating with the dental lab. A surgical guide is useful when placing multiple implants but not every patient will be suitable for surgically guided implants. A patient must have adequate architecture and bone volume in which to place the implants.
More helpful links:
Choosing the right type of surgical guide or safe guide »
Using guided surgery for restorative-driven implant treatment »
Using CAD/CAM surgical guides for a more successful implant surgery »
Advantages and benefits of computer-guided implant surgery »
CHAPTER VI: FULL ZIRCONIA IMPLANT RETAINED PROSTHESIS
Patients who are edentulous can often prove to be clinically challenging when deciding on the best type of implants and restoration. To avoid complications, it is necessary to fully understand the patient’s anatomy and to identify the volume of bone and vital structures that must be avoided for successful restoration with dental implants. The design will determine the number of implants required to achieve the correct occlusion and functionality while ensuring excellent esthetics. Given the advances in CAD/CAM technology and newer planning concepts, one of the best choices could be a full-arch zirconia implant retained bridge. This option has revolutionized fullarch rehabilitation and can provide patients with the opportunity to enjoy an incredibly natural smile that will restore functionality.
BENEFITS OF CHOOSING ZIRCONIA
Zirconia is a strong, versatile material that includes full-contour zirconia and layered zirconia. While full-contour zirconia can be an excellent choice for posterior teeth, layered zirconia can be used to closely replicate the appearance of anterior teeth. This type of full-arch bridge is highly resistant to fracturing and chipping, providing extremely good esthetics. It is also possible to achieve natural-looking gingival tissues with the use of layered ceramics. Additionally, only limited vertical space is required, providing a more conservative surgical option.
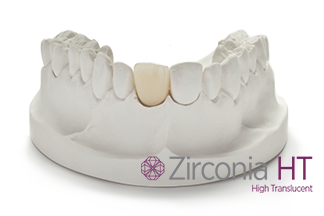
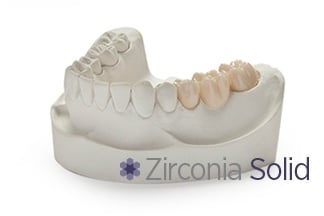
SCREW-RETAINED OR CEMENT-RETAINED?
Often, this type of prosthesis will be screw-retained because this allows for easier access during fitting and simple retrieval of the prosthesis. This also means it is straightforward to tighten the screws should the prosthesis become loose in any way. However, a cement-retained prosthesis ensures the occlusal surfaces are intact which may be esthetically preferable. Using CAD/CAM milling eliminates distortions that can occur during casting, producing a precision-fitting, cement retained prosthesis.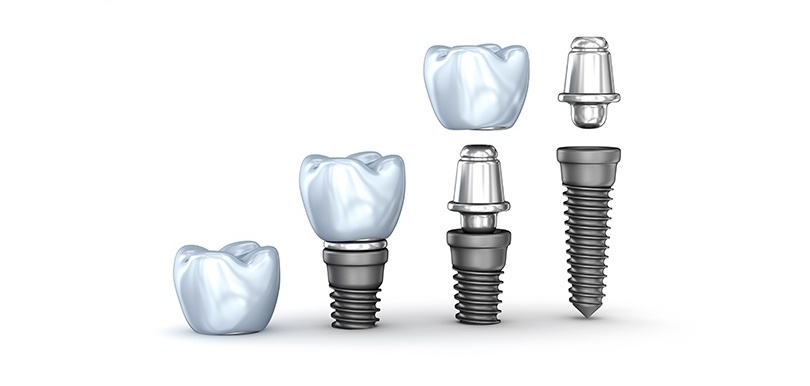
TREATMENT PLANNING
A CBCT is essential for treatment planning and ideally, a duplicate of the patient’s current denture or a diagnostic wax-up can be used during the scan to determine the position of the teeth to the underlying jawbone. The CBCT will also reveal any need for bone grafting and will determine the optimal angulation of the implants including the correct implant length and width. Ideally, the scan will also be utilized to create a surgical guide but even if this is not the case, the scan is still vital for achieving a good surgical outcome. It is also important to discuss durability, esthetics, and comfort with the patient and whether they will choose a shortened dental arch that requires fewer implants or if they are prepared for the additional expense involved with additional teeth. The need for gingival tissue replacement should also be considered and must be positioned in such a way that it will be covered by the patient’s lip whenever they smile. Often a functional prototype will be tried in and worn by a patient to verify the functionality and esthetics before the final restoration is fabricated. Doing so can also help provide the patient with a good spare prosthesis, just in case.
A full zirconia implant retained prosthesis is not the cheapest option but it can satisfy patient demands for teeth that feel completely normal and better esthetics.
More helpful links:
Factors to consider when recommending All-On-Four »
Treating edentulous patients with All-On-Four »
When to recommend implant overdentures »
Implant Bar Overdenture - A step-by-step guide »
Implant retained versus implant supported dentures »
Guided bone regeneration in implant dentistry »
Bone grafting materials in implant dentistry »
FINAL THOUGHT
Dental implants are perhaps one of the most exciting things to happen within dentistry during the past few decades. Implant technology is constantly changing and improving as implant companies continually search for even better solutions for tooth loss. However, the choice of implant systems and treatment options can be confusing. Selecting the right solution could mean all the difference between a satisfied and happy patient who will recommend your services to others, or an unhappy patient who requires many hours of clinical support to try to resolve the situation. It is also important to keep in mind that dental implants will not be the right option for everybody, and patients should be carefully screened for suitability before recommending dental implants.
Having the right dental laboratory to assist you with your dental implant treatments can be invaluable. Our experienced technical team is always willing to discuss any case with you and our in-depth technical knowledge will enable you to make the right treatment choices. We can liaise closely with you through the entire treatment, ensuring your patient is satisfied.